Ultrasonic Rhinoplasty
Piezo-assisted bone reshaping within contemporary rhinoplasty
Ultrasonic rhinoplasty uses piezoelectric instrumentation to work on the nasal bones with greater precision and soft-tissue preservation.
On this page, the term refers to piezo-assisted bone work as part of primary,
revision, functional and selected post-traumatic rhinoplasty planning.
Dr George Mireas
Primary Rhinoplasty
Revision Rhinoplasty
Preservation Rhinoplasty
3D Imaging & Simulation
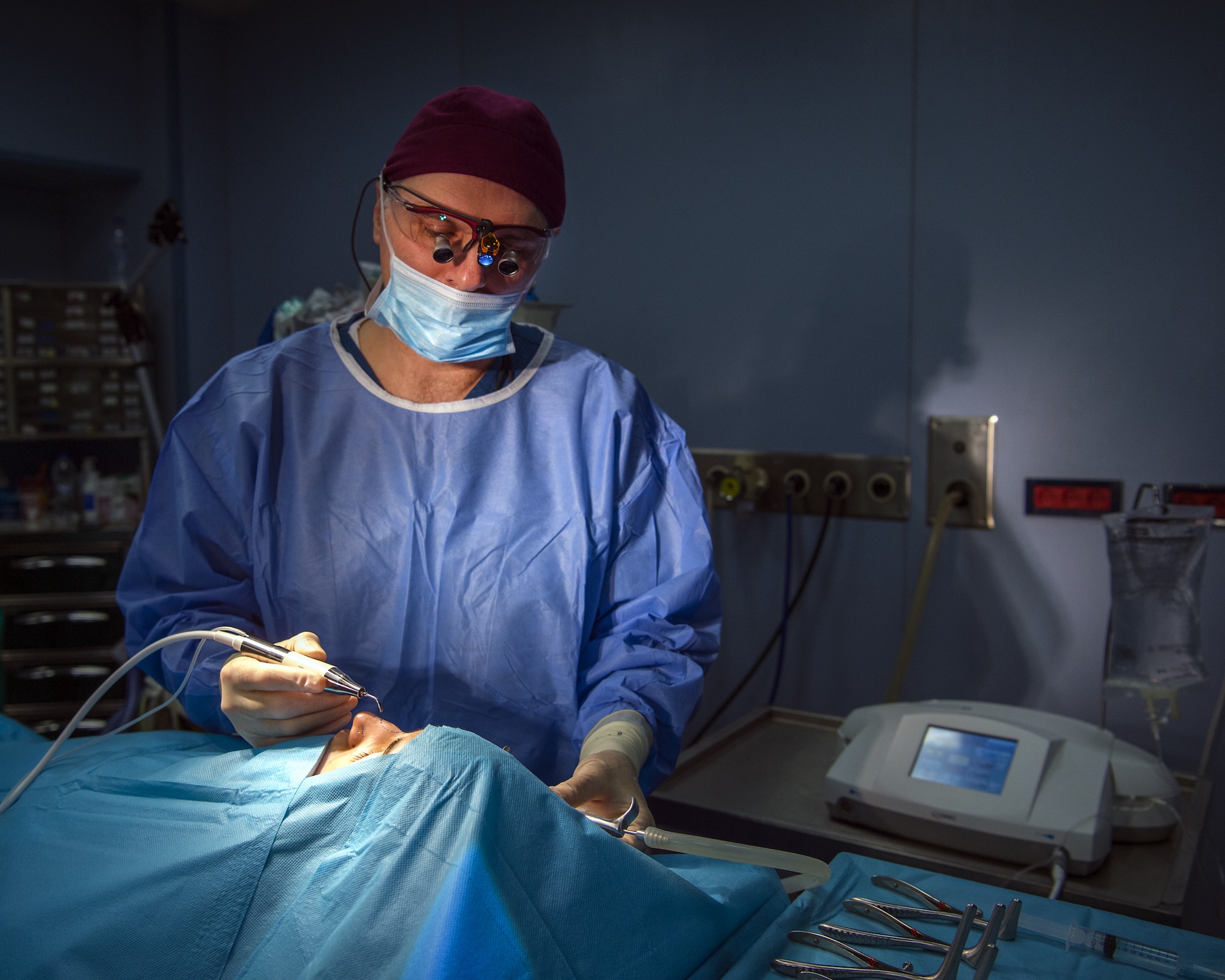
What Is Ultrasonic Rhinoplasty?
Ultrasonic rhinoplasty is a rhinoplasty technique in which piezoelectric instruments are used to work on the nasal bones with direct control and high precision.
Instead of relying only on conventional osteotomes, rasps or less controlled bone-cutting maneuvers, the surgeon can sculpt, thin, contour or selectively cut
the bony framework with greater accuracy.
In practical terms, this means that the bony part of rhinoplasty can often be performed in a more controlled way, with less trauma to soft tissues such as skin,
mucosa and vessels. This is particularly valuable when the goal is not only aesthetic refinement, but also structural precision and stable long-term support.
The Piezo System and Dedicated Microtips
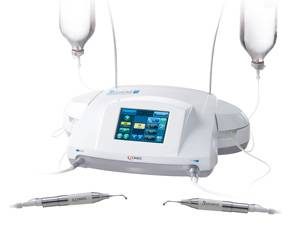
The Piezo System
The technology uses ultrasonic vibrations transmitted through specialized metallic tips designed for precise work on mineralized tissue.
These tips are intended to act on bone while minimizing collateral trauma to adjacent soft tissues. In rhinoplasty, this allows more refined control
during hump reduction, bony vault reshaping, narrowing of selected nasal bones and correction of asymmetries.
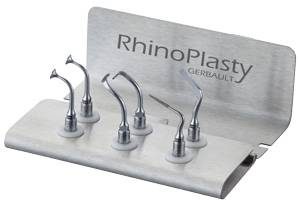
Piezo Microtips
One of the important advances of modern ultrasonic rhinoplasty is the availability of dedicated microtips that permit delicate and highly selective
work in the narrow anatomy of the nose. These tips make the technology far more useful in rhinoplasty than earlier, bulkier instruments and contribute
to the precision that distinguishes modern piezo-assisted surgery.
Clinical Advantages of Ultrasonic Rhinoplasty
The value of ultrasonic rhinoplasty is not that it replaces overall rhinoplasty planning. Its value is that it improves how certain parts of the operation can be executed.
Depending on the anatomy, this may allow:
- more precise work on the nasal bones under better control,
- more selective treatment of humps and bony irregularities,
- more refined narrowing or contouring in selected wide noses,
- reduced collateral trauma to surrounding soft tissues,
- less bruising and swelling in many patients,
- more predictable management of asymmetries in selected cases,
- useful application in selected revision and post-traumatic situations.
Why This Matters in Revision and Complex Cases
The bony part of revision rhinoplasty can be especially challenging.
Previous surgery may have left irregular healing, residual asymmetry, poorly positioned fractures or bones that are difficult to mobilize in a precise way.
In such situations, a more controlled technique can be particularly valuable.
Ultrasonic rhinoplasty may therefore play an important role when revision surgery requires careful modification of bone contours, correction of asymmetry
or management of prior osteotomy lines. It may also be relevant in selected post-traumatic cases where precision is especially important.
This does not mean piezo alone determines the outcome; revision rhinoplasty still depends on diagnosis, structural planning, graft strategy when needed
and extensive surgical experience.
Educational Video
A single explanatory video is sufficient here and fits the educational tone of the site.
Educational explanation of piezo-assisted bone work in rhinoplasty.
Who May Benefit
Ultrasonic rhinoplasty may be considered in selected patients undergoing:
- primary rhinoplasty involving significant bony vault work,
- revision rhinoplasty where controlled bone correction is needed,
- functional rhinoplasty combined with structural refinement,
- selected post-traumatic cases with asymmetry or irregular bone contours.
Whether it is the best option depends on the individual anatomy and on the overall surgical plan rather than on a single label or trend.
Ultrasonic Rhinoplasty Within the Broader Surgical Plan
Piezo-assisted bone work should always be understood within the broader structure of rhinoplasty planning. The quality of the result depends on diagnosis,
septal support, tip strategy, airway evaluation, skin characteristics and overall structural balance, not on one instrument alone.
For that reason, ultrasonic rhinoplasty is often best discussed together with the broader rhinoplasty framework,
especially in relation to primary rhinoplasty,
revision rhinoplasty and
preservation rhinoplasty.
Frequently Asked Questions
Is ultrasonic rhinoplasty a different operation from rhinoplasty?
No. It is a way of performing the bony part of rhinoplasty with piezoelectric instruments. It is best understood as a technique within rhinoplasty, not as a separate category of surgery.
Does every patient need piezo-assisted surgery?
No. Some patients benefit clearly from piezo-assisted bone work, while in others the main issues lie elsewhere, such as septal support, tip structure, skin thickness or graft strategy.
The operation should be designed around the patient rather than around the instrument.
Can ultrasonic rhinoplasty reduce bruising and swelling?
In many cases, yes. Better preservation of surrounding soft tissues may translate into less bruising and a smoother early recovery.
However, recovery still depends on the full extent of surgery and individual healing patterns.
Can ultrasonic rhinoplasty be useful in revision cases?
It may be particularly useful in selected revision cases where controlled bone work is necessary. That said, revision rhinoplasty remains a complex procedure whose success depends on the overall diagnostic and reconstructive plan.
Are the results permanent?
Rhinoplasty results are intended to be long-lasting. Long-term stability depends on the quality of the surgical plan, structural support, healing and the patient’s anatomy rather than on one instrument alone.
